
Dr Chong Wai KwongConsultant DermatologistsMBBS (Singapore), MRCP (UK), FRCP (Edinburgh), Dip Ven (London), FAMS (Dermatology)
Eczema and psoriasis are both common skin conditions that cause visible inflammation, discomfort and recurring flare-ups. They are often confused for one another due to overlapping chronic symptoms such as redness, itching, dryness and a scaly texture to the skin.
Despite these similarities, eczema and psoriasis are distinct conditions with different underlying mechanisms and treatment approaches. An accurate diagnosis by a dermatologist is important to help ensure the condition is correctly identified and managed with the most appropriate care.
Despite these similarities, eczema and psoriasis are distinct conditions with different underlying mechanisms and treatment approaches. An accurate diagnosis by a dermatologist is important to help ensure the condition is correctly identified and managed with the most appropriate care.
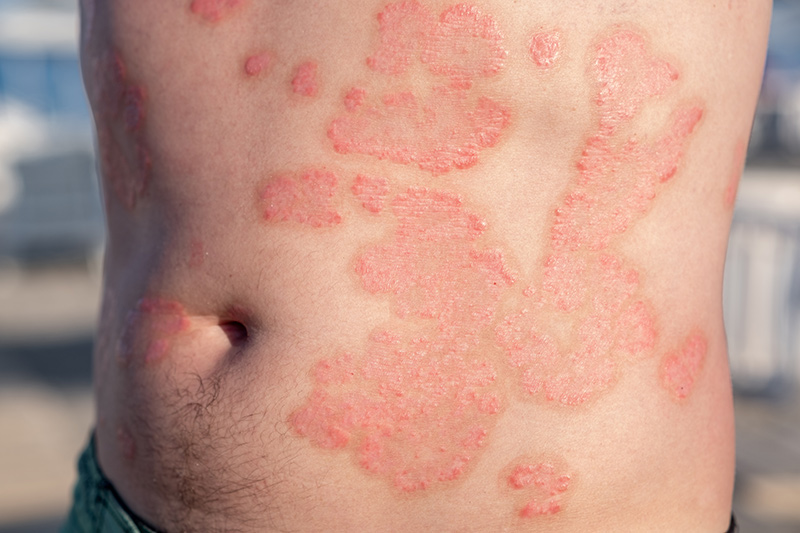
What is Eczema?
Eczema is a long-term inflammatory skin condition that affects the skin’s ability to retain moisture and protect itself from irritants and allergens. This weakened skin barrier leads to dryness, redness, itching, and, in some cases, cracking or oozing of the skin. Symptoms often appear in cycles, with periods of flare-ups followed by times of improvement. Eczema can affect people of all ages, though it commonly starts in childhood and may persist or recur later in life.
What is Psoriasis?
Psoriasis is a chronic immune-mediated skin condition that causes the rapid buildup of skin cells, leading to thickened, inflamed patches on the skin. These patches are often red and covered with silvery scales and they may cause itching, discomfort or pain. Psoriasis can develop at any age and tends to follow a relapsing pattern. It commonly affects areas such as the scalp, elbows, knees and lower back, though it can appear anywhere on the body.
How Eczema and Psoriasis Differ
Although eczema and psoriasis can look similar at first glance, several key features help distinguish one from the other. Understanding these differences can provide useful context before seeking a formal diagnosis.
● Primary Symptoms
Itching is a prominent feature of eczema and can be intense, often leading to scratching and skin damage. Psoriasis may also itch, but discomfort is more often described as burning, stinging or soreness rather than severe itching.● Appearance
Eczema typically presents as red, dry and inflamed skin with a rough or cracked surface and less well-defined edges. Psoriasis, in contrast, appears as thickened, raised plaques with clear borders and silvery or white scales.● Most Common Locations
Eczema commonly affects skin folds, such as the inner elbows, behind the knees, neck and wrists, though it can occur anywhere. Psoriasis more often involves the outer surfaces of the body, including the elbows, knees, scalp and lower back.● Triggers and Patterns
Eczema flare-ups are frequently linked to allergens, irritants, stress, weather changes and certain fabrics or skincare products. Psoriasis flares are more commonly associated with immune-related triggers, such as infections, stress, skin injury and allergic reactions to medications. Psoriasis may follow more defined flare–remission cycles instead of being triggered by outside stimuli like eczema.
How Dermatologists Can Tell Eczema and Psoriasis Apart
Dermatologists usually distinguish between eczema and psoriasis by conducting a detailed skin examination and reviewing the patient’s medical history. In some cases, additional tests may be needed to confirm the diagnosis or identify contributing factors. These may include:
- Skin Biopsy: A small sample of skin is examined under a microscope to clarify the diagnosis.
- Allergy Testing: Blood tests or skin-prick tests may be used to identify allergens that could trigger eczema flare-ups.
- Blood Tests: While not always necessary, these tests can help rule out other conditions or assess whether psoriasis-like symptoms are actually being caused by a disease.
- Patch Testing: Small patches containing common allergens are applied to the skin, usually on the back, for about 48 hours. This helps identify substances that may cause allergic contact dermatitis, especially in eczema.
When Should I Visit a Dermatologist for Skin Flare-Ups?
It may be time to see a dermatologist if skin flare-ups become persistent, progressively worse or difficult to manage on your own. This is especially true if you cannot determine whether your condition is eczema or psoriasis. Seeing a dermatologist is recommended when:
- You are unsure whether the condition is eczema, psoriasis or another skin disorder
- Red, inflamed or scaly patches do not improve with over-the-counter treatments
- Itching, discomfort or pain is severe or affecting daily life
- Skin symptoms appear suddenly, spread quickly or are accompanied by signs of infection (such as pus, swelling or warmth)
- Home care or lifestyle changes fail to prevent flare-ups
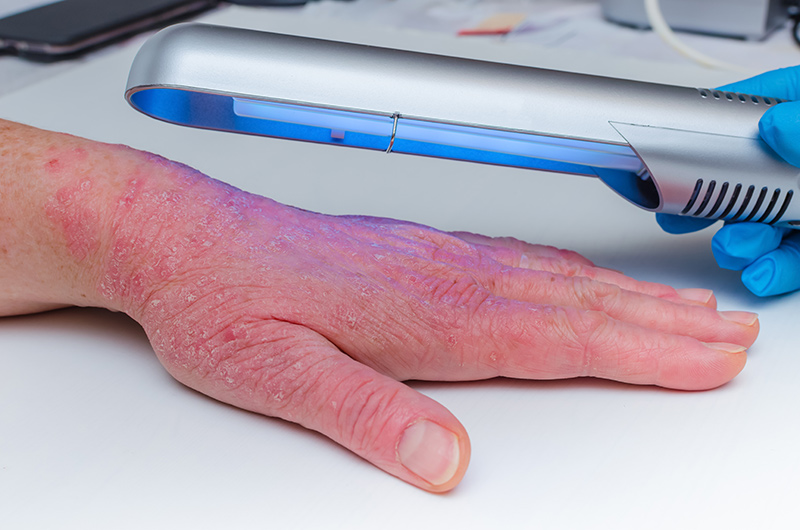
At Specialist Skin Clinic, we provide structured, dermatologist-led management tailored to your specific type of skin condition. Management focuses on careful evaluation, evidence-based treatment planning and regular follow-up to support sustained control. Under the care of consultant dermatologist Dr Cheong Wai Kwong, we offer treatment for eczema and other skin conditions across all age groups, including more complex or treatment-resistant cases.
If you are seeking eczema care in Singapore, contact-us, today to schedule an appointment.
If you are seeking eczema care in Singapore, contact-us, today to schedule an appointment.
With appropriate treatment, it is entirely possible to lead a good quality of life with eczema.
We welcome you to drop by for a detailed and personalised assessment.
Thank you for choosing Specialist Skin. Please fill up the form below and we will get back to you as soon as possible.

1 Grange Road #06-04, Orchard Building,
Singapore 239693
Singapore 239693
Mon - Fri : 8:30am - 5:00pm
Sat : 8:00am - 1:00pm
Sat : 8:00am - 1:00pm
Closed on Sundays and public holidays
Blogs