
Dr Chong Wai KwongConsultant DermatologistsMBBS (Singapore), MRCP (UK), FRCP (Edinburgh), Dip Ven (London), FAMS (Dermatology)
Severe eczema goes far beyond the occasional itching. It is often persistent, widespread, intense and prone to flare-ups that disrupt sleep, work and your daily routine. In these cases, specialist aid is often necessary in order to alleviate these symptoms and restore your quality of life.
Dermatologists may treat moderate to severe eczema using a structured, medical approach that aims to address skin inflammation, restore the skin barrier and reduce the frequency and severity of flares. This could involve prescription medicine, targeted skin treatment or other long-term management plans tailored to individual patients, depending on the severity of their symptoms.
Dermatologists may treat moderate to severe eczema using a structured, medical approach that aims to address skin inflammation, restore the skin barrier and reduce the frequency and severity of flares. This could involve prescription medicine, targeted skin treatment or other long-term management plans tailored to individual patients, depending on the severity of their symptoms.
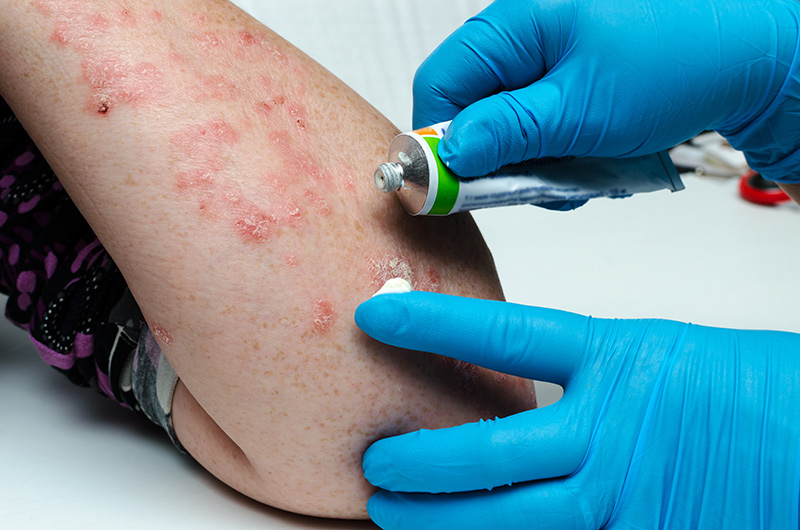
Assessing Eczema Severity
Dermatologists often begin the treatment process by carefully assessing the severity of eczema. This involves evaluating how much of the skin is affected, the intensity of itching, the frequency of flare-ups and the impact on sleep and daily quality of life. Clinical judgement is often supported by validated scoring systems to classify eczema as mild, moderate or severe.
Common tools used to assess eczema severity include:
Common tools used to assess eczema severity include:
- Eczema Area and Severity Index (EASI): This tool measures the extent of eczema and grades features such as redness, thickness, scratching and skin changes across different body regions.
- Scoring Atopic Dermatitis (SCORAD): SCORAD assesses the area of skin involved, the intensity of visible symptoms and patient-reported factors such as itch and sleep disturbance.
- Investigator’s Global Assessment (IGA): IGA is a simplified scale in which the dermatologist rates overall eczema severity, ranging from clear skin to severe disease, based on clinical appearance.
Once these tools have been utilised, your dermatologist will likely be able to conclude whether your eczema is mild, moderate or severe.
Topical Medical Treatments for Moderate To Severe Eczema
Dermatologists usually begin treatment of eczema by using topical treatment. This step forms the foundation of eczema management. In moderate to severe cases, prescription-strength topical therapies are often needed to control inflammation, relieve itching and support skin barrier repair. These treatments are more targeted than those used for mild eczema.
Common topical treatment options include:
Common topical treatment options include:
- Moderate- to High-Potency Topical Corticosteroids: These medications reduce inflammation and redness during active flares. The choice of strength and duration is carefully adjusted based on the affected area, the patient’s age and disease severity.
- Topical Calcineurin Inhibitors: These non-steroidal creams or ointments help control inflammation. They are commonly used on sensitive areas such as the face, neck or skin folds, and may be suitable for longer-term management.
- Topical PDE-4 Inhibitors: These treatments work by reducing inflammatory signals in the skin. They may be considered for patients who cannot tolerate topical steroids or who require steroid-sparing options.
- Topical JAK Inhibitors: These newer therapies target specific inflammatory pathways involved in eczema. They are used in selected moderate to severe cases under close medical supervision.
- Medicated Emollients and Barrier Repair Creams: These products play a key role in restoring the skin barrier. Regular use helps improve skin hydration and enhances the effectiveness of anti-inflammatory treatments.
Throughout this process, your dermatologist closely monitors each step and helps ensure phototherapy is delivered safely.
Advanced Therapies for Severe Eczema
For individuals with severe eczema, symptoms can be difficult to control despite consistent treatment and skincare. Ongoing inflammation, frequent flare-ups and significant impact on quality of life often signal the need for a more specialised level of management. In these cases where standard approaches are insufficient, your dermatologist may recommend more complex options that include:
1. Phototherapy (Light Therapy)
Phototherapy involves exposing the skin to controlled doses of ultraviolet light under medical supervision. It helps reduce inflammation, relieve itching and slow down abnormal skin cell growth. Phototherapy is especially useful for patients with eczema covering large areas of the body or for those who cannot tolerate long-term use of strong topical medications.
2. Systemic Therapies
Systemic treatments work from within the body to control the immune response that drives eczema. They are prescribed for severe or treatment-resistant cases. Options include:
- Oral immunosuppressants, such as cyclosporine and methotrexate, that dampen overall immune activity to reduce inflammation.
- Biologic therapies, such as dupilumab, that specifically target immune pathways involved in eczema flare-ups, offering more precise control over your skin with fewer systemic effects.
3. Combination Therapy
In many cases, dermatologists continue topical treatments alongside phototherapy or systemic medications. This combined approach enhances effectiveness, protects the skin barrier and helps maintain long-term control.
How Can I Manage Eczema Through Lifestyle Changes?
Treatment for moderate or severe eczema can be supported by careful management of triggers and daily lifestyle habits. Making small, consistent changes may help reduce flare-ups and support healthier skin over time.
Helpful steps include:
Helpful steps include:
- Maintaining a Regular Skincare Routine: Apply moisturisers and emollients daily to keep the skin hydrated and protect the skin barrier.
- Avoiding Personal Triggers: Identify and limit exposure to irritants such as harsh soaps, fragrances, certain fabrics or known allergens that may worsen symptoms.
- Managing Stress: Stress can trigger or worsen eczema. Relaxation techniques, gentle exercise or mindfulness practices may help reduce flare frequency.
- Prioritising Good Sleep: Adequate, restful sleep supports skin repair and overall immune health.
- Supporting Skin Health Through Diet and Hydration: Eating a balanced diet and drinking enough fluids can help maintain overall well-being, which may positively influence skin condition.
Monitoring and Follow-Up Care After Eczema Treatment
For moderate to severe eczema, regular monitoring and follow-up care are important for maintaining long-term control and reducing the risk of complications.
Dermatologists schedule ongoing reviews to assess how well treatments are working, monitor changes in symptoms and adjust management plans when needed. These visits help determine whether topical therapies, phototherapy or systemic medications remain appropriate, and whether treatment doses or combinations should be modified. Follow-up care also allows for early detection of side effects, supporting safe and effective long-term management.
Dermatologists schedule ongoing reviews to assess how well treatments are working, monitor changes in symptoms and adjust management plans when needed. These visits help determine whether topical therapies, phototherapy or systemic medications remain appropriate, and whether treatment doses or combinations should be modified. Follow-up care also allows for early detection of side effects, supporting safe and effective long-term management.
Moderate To Severe Eczema Treatment at Specialist Skin Clinic
If you or a family member has recurrent or widespread eczema that disrupts sleep or daily life, a dermatology assessment may help identify suitable treatment options and improve long-term control. At Specialist Skin Clinic, we are experienced in managing eczema across all age groups and severity levels, including complex and treatment-resistant cases.
Under the care of consultant dermatologist Dr Cheong Wai Kwong our approach emphasises accurate diagnosis, trigger identification and evidence-based management. Assessments may include eczema severity scoring, tailored treatment planning and evaluation for advanced therapies where appropriate.
Under the care of consultant dermatologist Dr Cheong Wai Kwong our approach emphasises accurate diagnosis, trigger identification and evidence-based management. Assessments may include eczema severity scoring, tailored treatment planning and evaluation for advanced therapies where appropriate.
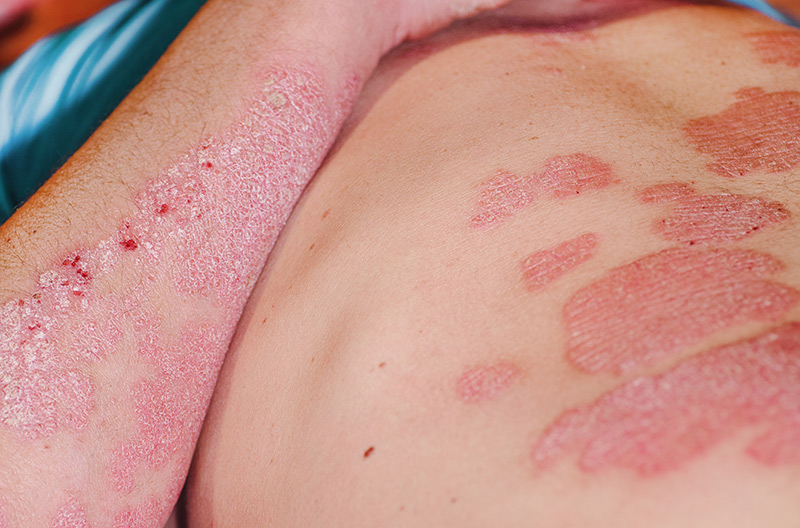
If you are seeking eczema care in Singapore, contact-us, today to schedule an appointment.
With appropriate treatment, it is entirely possible to lead a good quality of life with eczema.
We welcome you to drop by for a detailed and personalised assessment.
Thank you for choosing Specialist Skin. Please fill up the form below and we will get back to you as soon as possible.

1 Grange Road #06-04, Orchard Building,
Singapore 239693
Singapore 239693
Mon - Fri : 8:30am - 5:00pm
Sat : 8:00am - 1:00pm
Sat : 8:00am - 1:00pm
Closed on Sundays and public holidays
Blogs